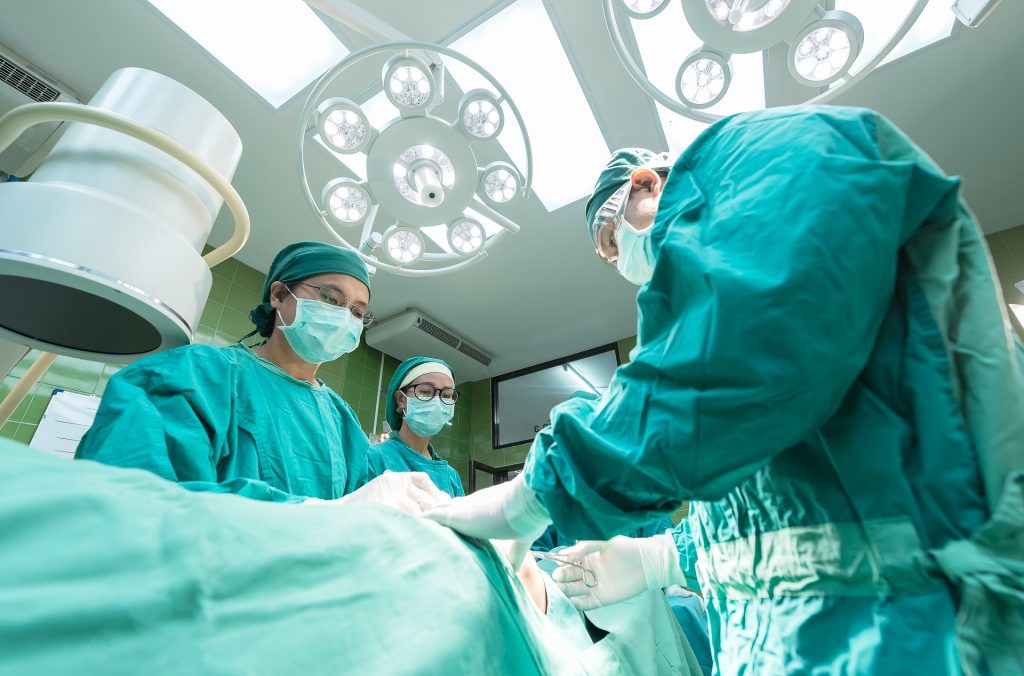
For most pet cancers, surgery is the primary form of treatment. Surgery is used to remove or reduce the size of a tumour and make any subsequent treatments with chemotherapy and/or radiation therapy, more effective.
In some cases, chemotherapy or radiation therapy is used before surgery to shrink the tumour so it’s easier to remove. Sometimes surgery is performed to increase a pet’s quality of life or make them more comfortable such as amputating a limb for pets with osteosarcoma or removing the spleen in a pet with hemangiosarcoma to prevent internal bleeding.
For some pets, surgery offers a cure for cancer and for others, surgery offers a chance at an improved quality of life and longer survival times.
As with any serious medical procedure, the veterinarian will run a series of tests to ensure the pet is healthy enough to undergo surgery. These tests may include blood work; x-rays and/or ultrasound to determine if the cancer has spread to other organs; and other tests specific to the type of cancer involved.
During surgery, the veterinarian will remove the tumour as well as some of the normal tissue surrounding the tumour, called the “margin”, to ensure that all tumour cells have been removed. If the surgeon is unable to achieve “clean margins” (removal of all the cancer cells), then a second surgery may be performed and/or chemotherapy and/or radiation therapy are used to help destroy any remaining cancer cells.
If the cancer has spread to the local lymph nodes (which have the capacity to carry cancer cells to other organs in the body), these will likely be removed at the same time as the tumour.
Sometimes with large tumours, vets will use a surgical technique called debulking, which reduces the tumour to boost the chances of chemotherapy or radiation therapy working. If the pet undergoes chemotherapy or radiation therapy after surgery, there is usually a short waiting period to allow the dog to fully recover from the operation.
There are always risks associated with cancer surgery and those risks will vary depending on the type of surgery performed. For example, pet’s with osteosarcoma who have a limb amputated may experience post-surgery complications including phantom limb pain (the severed nerve thinks the limb is still there), seromas (build up of fluid at the surgical site) or a post-surgery blood clot.
Many pet parents express concern about putting their pets under general anaesthesia. Compared to other procedures, the risk of a reaction to anaesthesia is relatively low. Vets estimate that about one in 100,000 pets have a reaction to anaesthesia, and this can range from minor reactions such as swelling at the injection site to life-threatening reactions like anaphylactic shock.
Veterinarians take great care to minimize the risk to your pet by following strict anaesthesia protocols and carefully monitoring your pet while under anaesthesia and after surgery.
Source:
This page has been reviewed by our Panel of Experts for accuracy. Our Panel of Experts is comprised of practitioners with varying specialties and perspectives. As such, the views expressed here may not be shared by all members of our Panel.
The content on this website is for informational purposes only and is not intended to be a substitute for professional veterinary medical advice, diagnosis or treatment.